Ensuring effective employee healthcare management, is a strategic priority for companies. Between reimbursement tracking, pre-authorisation requests and access to medical benefits, traditional processes often remain complex and time-consuming, both for beneficiaries and HR teams.
To address these challenges, OLEA has launched the OLEA Health mobile app, designed to centralise and simplify all information related to employees’ health coverage. Its objective: To provide beneficiaries with a seamless and secure experience, while reducing the administrative burden for companies.
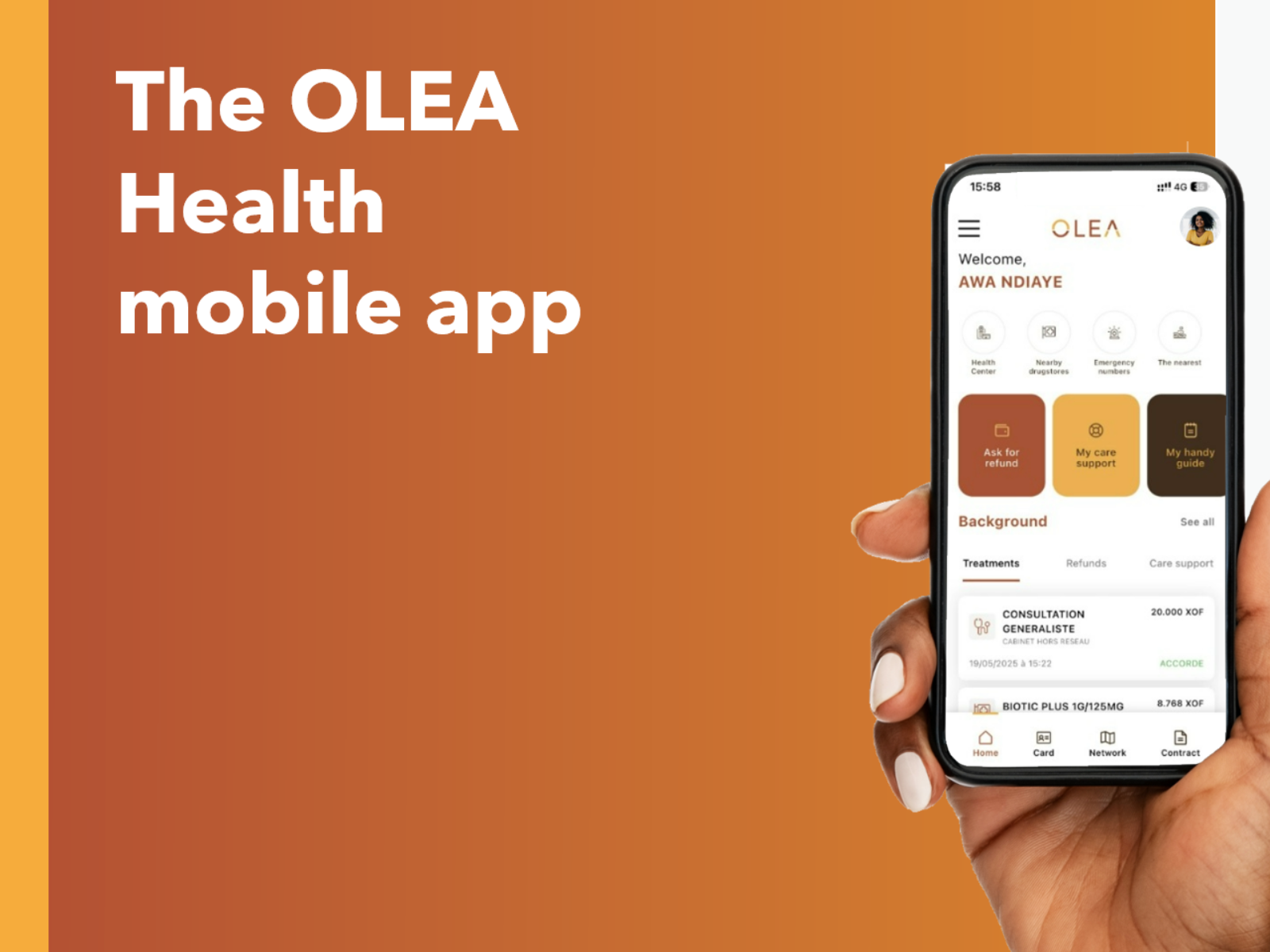
An app designed to make employees’ lives easier
Developed to make every interaction simpler and faster, the OLEA Health mobile app brings together essential features that enable beneficiaries to manage their healthcare coverage efficiently on a daily basis by:
- Real-time reimbursement tracking
- Access to coverage details and medical benefits
- Access to the partner healthcare network
- Beneficiary management, including dependents
- A digital health card, which is easily accessible
- Direct pre-authorisation requests by using the app to accelerate processes
- Rapid access to pharmacies, emergency numbers and healthcare facilities
- Enhanced security through multi-factor authentication
- Multilingual version: French, English and Portuguese
The strategic impact for the company
Beyond improving the employee experience, this app serves as a genuine optimisation lever for HR teams. The solution reduces administrative workload, limits the risk of errors and enables resources to refocus on employee support and well-being.
It is also integrated into OLEA’s pan-African third-party payment network, currently operational in 13 countries across West and Central Africa*. For companies operating in multiple countries, this means that an employee based in Côte d’Ivoire and traveling on assignment to Senegal, for example, can receive cashless medical treatment within the local partner network, while headquarters retains clear and centralised visibility through the App. This continuity of service ensures health cover is assured during business travel and strengthens the consistency of healthcare schemes for regional groups.
As highlighted by one of our HR clients in the logistics and catering sector: “The OLEA Health app is very easy to use. It allows me to track my reimbursements in real time and submit my invoices easily, wherever I am. The monitoring of my requests is clear and fast, which facilitates the efficient
management of my healthcare coverage significantly.”
To learn more about the OLEA Health offering and enable your employees to access the app upon subscription, please contact us at: ib.sy@olea.africa
*The OLEA Health pan-African third-party payment network is currently available in the following countries:
Benin, Burkina Faso, Cameroon, Central African Republic, Chad, Congo, Côte d’Ivoire, Gabon, Guinea, Mali, Niger, Senegal, and Togo.